# Principles of Allocation
## Overview
Our modern societies have chosen to develop medical systems in which only a limited amount of resources - such as nurses and physicians, treatment, equipment, and money - are available. Even in seemingly normal times, patients are triaged in the emergency room based on the urgency of their complaint and the availability of clinicians. In the current COVID-19 pandemic, the limitations in our medical resources as a nation and globally have become increasingly apparent, as we hear about shortages of essential equipment for patients and providers such as surgical and N95 masks, beds, and ventilators. As such, determining the allocation of medical resources has become a pressing topic for all. We provide a framework that incorporates basic principles of medical ethics (autonomy, justice, beneficence, and nonmaleficence) and guides decision-making regarding resource allocation (i.e. “rationing”).
## Framework
Based on the principles of autonomy, justice, beneficence, and nonmaleficence, [Persad et al. (2009)](https://www.thelancet.com/journals/lancet/article/PIIS0140-6736\(09\)60137-9/fulltext) propose four categories of ethical values to guide the allocation of scarce medical resources:
1\) treating people equally\
2\) giving priority to the worst off\
3\) maximizing benefits\
4\) promoting and rewarding social usefulness ([Persad et al. Lancet 2009](https://www.thelancet.com/journals/lancet/article/PIIS0140-6736\(09\)60137-9/fulltext)).
Within each category of ethical value, there are two competing ethical principles (for a total of eight sub-principles) that are competing specifications of the higher-order ethical value.
* **Treating people equally:** Allowing people to have equal opportunity to receive a medical intervention underlies this ethical value. This ethical value forms the basis for the following two principles, though they reach different conclusions:
* **Lottery (Random Selection):** This ethical principle uses a lottery to provide people with an equal probability of obtaining a given medical resource, regardless of other circumstances.
* **First-come, first-served:** Under this ethical principle, people who require a limited resource first receive it, without regard to differences between people. For example, during non-pandemic times, patients are allotted hospital beds on a first-come, first-served basis.
* **Giving priority to the worst off:** This ethical value embodies prioritarianism (see above), in which individuals who are worse off are given priority access to needed medical resources. Below, we discuss ethical principles that incorporate this ethical value, though they differ in their definition of who is considered worst off. While these principles are among the most discussed, they are not the only ones. There are multiple other ways of defining who is “worse off.”
* **Sickest first:** In this ethical principle, those with the worst chance of survival without a given scarce medical intervention are prioritized, as they are considered to be “worst off.”
* **Youngest first:** This ethical principle prioritizes the distribution of resources to those who have lived fewer life years - thus defining those who are “worst off” as those who have yet to benefit from having lived longer.
* **Maximizing benefits:** This ethical value is based upon utilitarianism (see above for detailed background on utilitarianism) and, at its core, aims to maximize the possible good that can be done. There are multiple ways, however, to define a “benefit,” and different ethical principles differ in the “benefit” that they promote. Two ethical principles falling under this ethical value are described below.
* **Saving the most lives:** This ethical principle prioritizes saving the most individual lives. It treats each life as holding equal value and does not compare the worth of each individual life - for example, the lives of a 20-year-old and 70-year-old are weighed equally.
* **Saving the most life-years:** In this ethical principle, saving the most life-years is preferred over saving the most lives, regardless of how this distribution is concentrated or spread. For example, this ethical principle would favor saving one person who goes on to live an additional 21 years rather than 20 people who each go on to live one additional year (20 life-years). There are multiple ways in which life years are quantified (see below).
* **Promoting and rewarding social usefulness:** This ethical value prioritizes people who have previously provided or will provide, in the future, benefit to society. It is important to recognize the effect that culture and societal norms have on defining these benefits to society and, thus, who would be prioritized.
* **Instrumental value:** In this ethical principle, people who have future usefulness are prioritized. For example, a system valuing instrumental value could focus on treating healthcare workers in the current COVID-19 pandemic because of the added value they may have for treating others in the future.
* **Reciprocity:** This ethical principle prioritizes and rewards people who previously were useful or had to sacrifice. In this system, a person who previously volunteered to test a new COVID-19 vaccine in a clinical trial would be prioritized if they were to require treatment in the future.
An important concept to understand within the context of the allocation of scarce resources (i.e. rationing) is the “life-year,” as it underlies the ethical principle of “saving the most life-years” in order to maximize benefits. There are [two general systems](https://nccid.ca/publications/understanding-summary-measures-used-to-estimate-the-burden-of-disease/) used to quantify life-years.
* **Quality-adjusted life-year:** Quality-adjusted life-year systems measure the gain of equivalent healthy years. In this system, a quality-adjusted life-year (QALY) is defined as one year of perfect health. A year of life with a specific illness or disability (i.e. health-related quality-of-life; HRQOL) is then normalized relative to this year of perfect health. Specific criteria for determining this normalized value vary, especially given the subjective nature of the “value” of a specific condition. For example, in the UK’s National Health Service, a year of life with a moderate mobility impairment is defined as 0.85 QALYs.
* **QALYs formula: QALYs = additional years of life x health-related quality-of-life (HRQOL)**
* **Disability-adjusted life-year:** Disability-adjusted life-year systems measure the loss of health. This system measures the total length of time that a specific illness is disabling to an individual over their lifetime. Similar to a QALY, it incorporates quality-of-life factors to normalize a year of living with a specific condition/illness to a year of perfect health. Prior DALY systems included an age-weighting such that a year for a younger person was weighed as more valuable than that for an older person, but these weightings have generally since been removed.
* **DALYs formula: DALYs = years of life lost to premature mortality (YLL) + years lived with disability (YLD)**
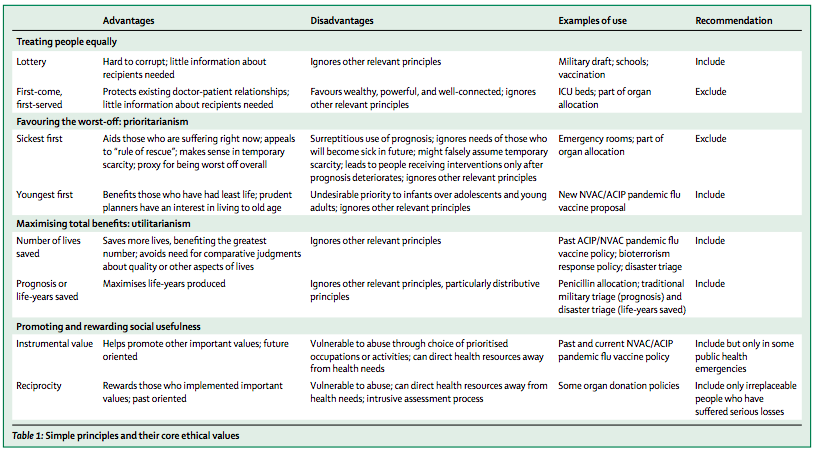
Each of these ethical values and principles has advantages and disadvantages (summarized in Table 1 below). [Persad et al. (2009)](https://www.thelancet.com/journals/lancet/article/PIIS0140-6736\(09\)60137-9/fulltext) have also developed a recommendation as to whether each ethical principle should be included or excluded when developing guidelines for allocation.
When developing a framework for allocation of scarce resources, it is important to recognize that no single value or principle is sufficient in determining whether a given individual receives the resource. Ultimately, a multi-value and multi-principle framework is necessary to facilitate such decision-making ([Emanuel et al. NEJM 2020](https://www.nejm.org/doi/full/10.1056/NEJMsb2005114)).
Similar to [Persad et al. (2009)](https://www.thelancet.com/journals/lancet/article/PIIS0140-6736\(09\)60137-9/fulltext), [White and colleagues (2009)](https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2629638/) suggest a framework for the allocation of scarce medical resources that include maximizing life-years, broad social value, instrumental value, and the life-cycle principle (i.e. providing each individual with an equal opportunity to live through various stages of life). ([Who Should Receive Life Support During a Public Health Emergency? Using Ethical Principles to Improve Allocation Decisions](https://annals.org/aim/article-abstract/744219/who-should-receive-life-support-during-public-health-emergency-using)). However, they caution against over-reliance on maximizing life-years, as this practice may selectively discriminate against groups with certain conditions. For example, maximizing life-years could lead to favoring the lives of those who are younger and able-bodied, while disadvantaging those who are older and have disability. Please see [vulnerable populations below](https://docs.google.com/document/d/1eqtWy5fS_qd_e8jM58ii9wUr8_npHaVLPF-mHmqFvsg/edit#bookmark=id.lkprh7i1862w) for further discussion.
Although the above ethical values and principles for medical resource allocation suggested by [Persad et al. (2009)](https://www.thelancet.com/journals/lancet/article/PIIS0140-6736\(09\)60137-9/fulltext) are well-known, there are others as well. Some advocate for the interrelated concepts of cost, opportunity costs, and cost effectiveness to be considered within the principles of allocation. [Sheehan and Hope (2002)](https://books.google.com/books?hl=en\&lr=\&id=YsQIbtX2GXsC\&oi=fnd\&pg=PP1\&ots=BTE5i-2BrB\&sig=1tYGM2hagkyrf_joKZ7C0wF2mDE#v=onepage\&q\&f=false) in Allocating Health Care Resources in the UK promote this approach. Because cost is a limiting factor in medical budgets, they argue that it is important to assess the relative opportunity costs of approaches to allocation, as funding one area means another area will not receive funding. As such, cost effectiveness can be an essential consideration in deciding medical resource allocation. This approach to cost effectiveness is not solely limited to the hospital or medical center setting, but instead applies to society more broadly. For instance, during an economic downturn, we use cost effectiveness when deciding where to direct stimulus money (hospital vs. industry vs. directly to families).
*Thought Questions:*
* If you were developing a system of allocation for your country, which principles would you weigh most heavily and/or least heavily, and why?
* What role should monetary cost have in guiding decisions within an allocation system?
* What decisions (societal, governmental, personal, etc.) have been made in the past that have now caused rationing to be necessary in the setting of scarcity?
* Are there solutions outside of rationing that can solve the scarcity of medical resources?
**References:**
* [Emanuel, Ezekiel J., et al. "Fair allocation of scarce medical resources in the time of Covid-19." (2020).](https://www.nejm.org/doi/full/10.1056/NEJMsb2005114)
* [Persad, Govind, Alan Wertheimer, and Ezekiel J. Emanuel. "Principles for allocation of scarce medical interventions." The Lancet 373.9661 (2009): 423-431.](https://www.thelancet.com/journals/lancet/article/PIIS0140-6736\(09\)60137-9/fulltext)
* NCCID. “Understanding Summary Measures Used to Estimate the Burden of Disease: All about HALYs, DALYs and QALYs”. (2015)
* [Sheehan, M., and T. Hope. "Allocating healthcare resources in the UK: putting principles into practice." Medicine and social justice: essays on the distribution of healthcare (2002): 219-230.](https://books.google.com/books?hl=en\&lr=\&id=YsQIbtX2GXsC\&oi=fnd\&pg=PP1\&ots=BTE5i-2BrB\&sig=1tYGM2hagkyrf_joKZ7C0wF2mDE#v=onepage\&q\&f=false)
* [White, Douglas B., et al. "Who should receive life support during a public health emergency? Using ethical principles to improve allocation decisions." Annals of Internal Medicine 150.2 (2009): 132-138.](https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2629638/)
---
# Agent Instructions: Querying This Documentation
If you need additional information that is not directly available in this page, you can query the documentation dynamically by asking a question.
Perform an HTTP GET request on the current page URL with the `ask` query parameter:
```
GET https://curriculum.covidstudentresponse.org/module-8-medical-ethics/principles-of-allocation.md?ask=
```
The question should be specific, self-contained, and written in natural language.
The response will contain a direct answer to the question and relevant excerpts and sources from the documentation.
Use this mechanism when the answer is not explicitly present in the current page, you need clarification or additional context, or you want to retrieve related documentation sections.