# Personal Protective Equipment
## What is PPE?
Personal protective equipment (PPE) is designed to protect the wearer from illness or injury due to contact with occupational hazards, such as dangerous chemicals, radioactive materials, or infectious biological agents. PPE may include items such as gloves, goggles, shoe covers, helmets, respirators, masks, gowns, or full body suits ([Occupational Safety and Health Administration](https://www.osha.gov/SLTC/personalprotectiveequipment/)).
## Importance of PPE
Medical professionals commonly use PPE in the inpatient and outpatient settings, as well as in clinical laboratories. Correct use successfully creates a barrier between the wearer’s skin and potentially infectious materials such as patients’ bodily fluids, thereby stopping transmission of bacterial or viral pathogens. Patients at high risk for contracting infections, such as those with significant cardiopulmonary comorbidities or an immunodeficiency, can also use PPE to protect themselves from exposure to infectious agents brought in by visitors or healthcare workers. Correct use of PPE, in combination with other infection control practices (e.g. washing hands, using alcohol-based hand sanitizers, covering coughs and sneezes), reduces the spread of infection ([FDA](https://www.fda.gov/medical-devices/general-hospital-devices-and-supplies/personal-protective-equipment-infection-control)).
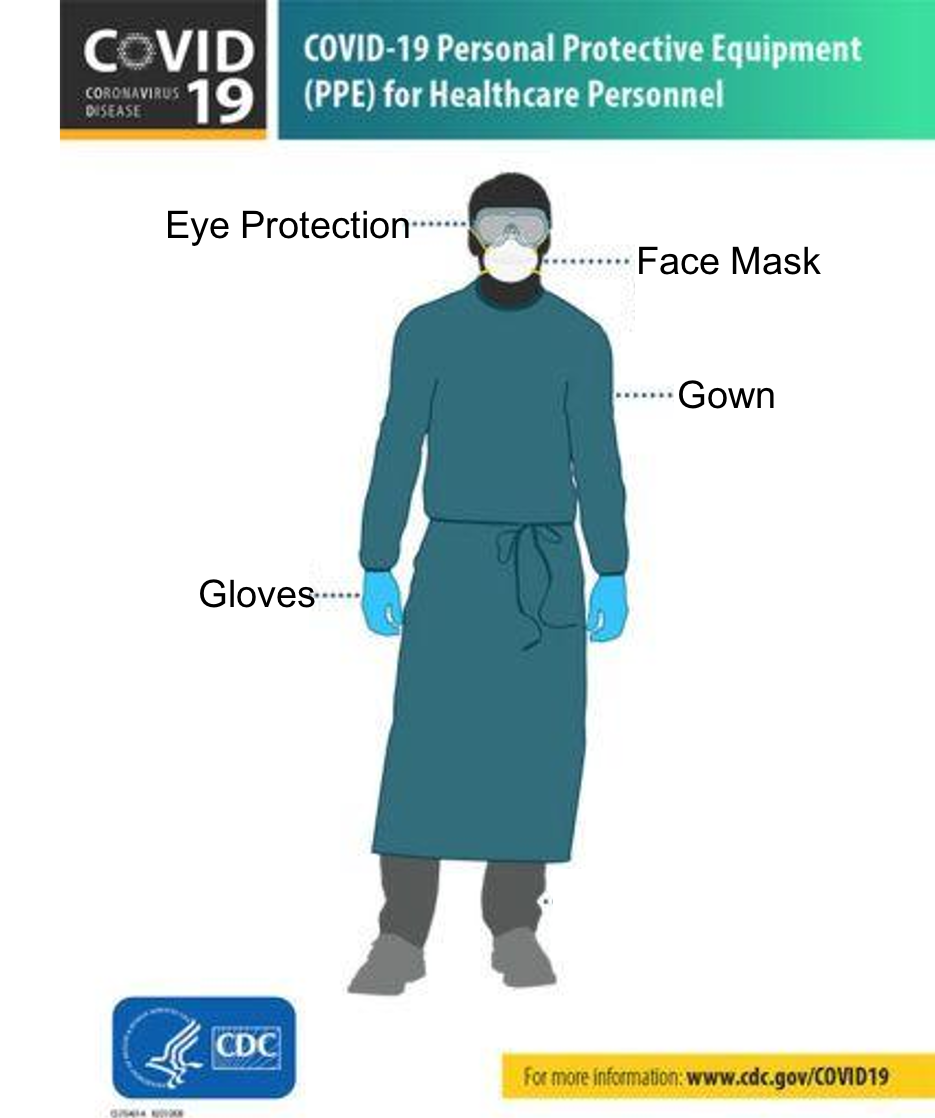
The [CDC](https://www.cdc.gov/coronavirus/2019-ncov/hcp/respirator-use-faq.html) provides clear guidelines concerning the selection and use of PPE in healthcare settings for both patients and healthcare personnel. Significantly, staff caring for patients with confirmed or suspected COVID-19 should wear a gown, gloves, eye protection, and a mask. Currently, many institutions are reserving N95 masks for aerosolizing procedures due to the limited stock.
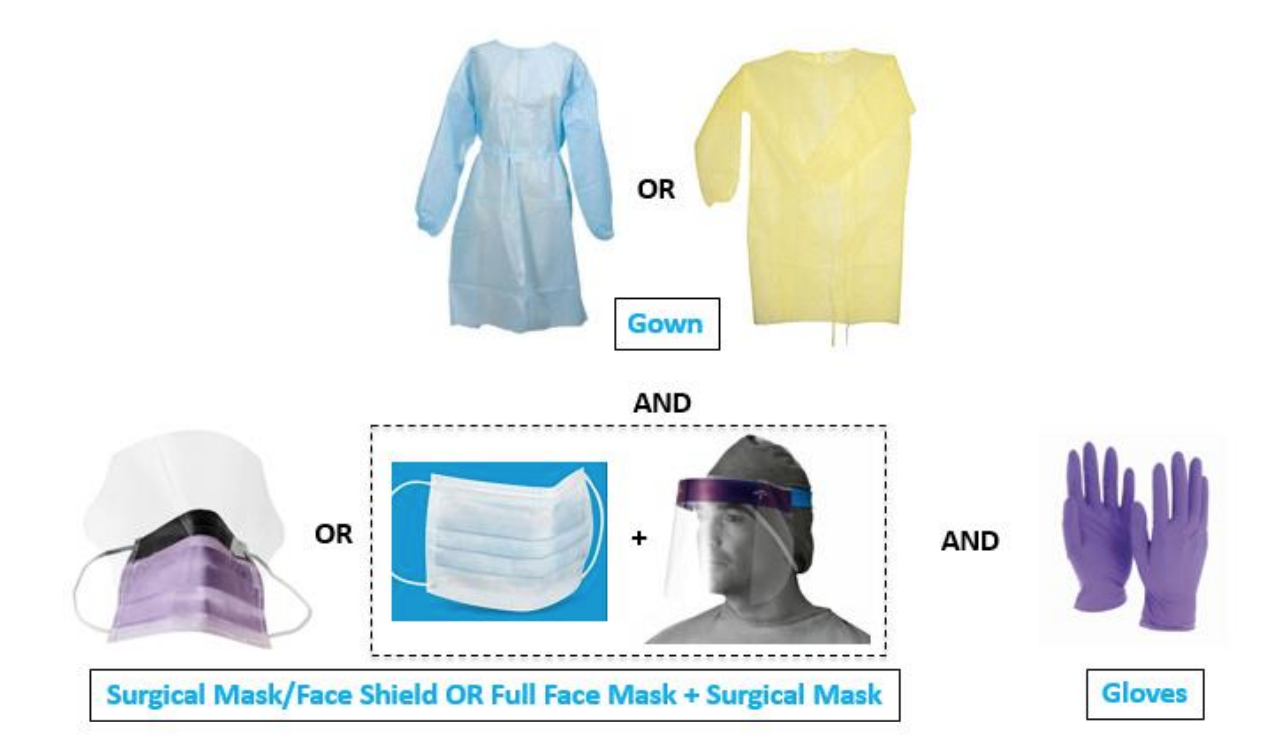
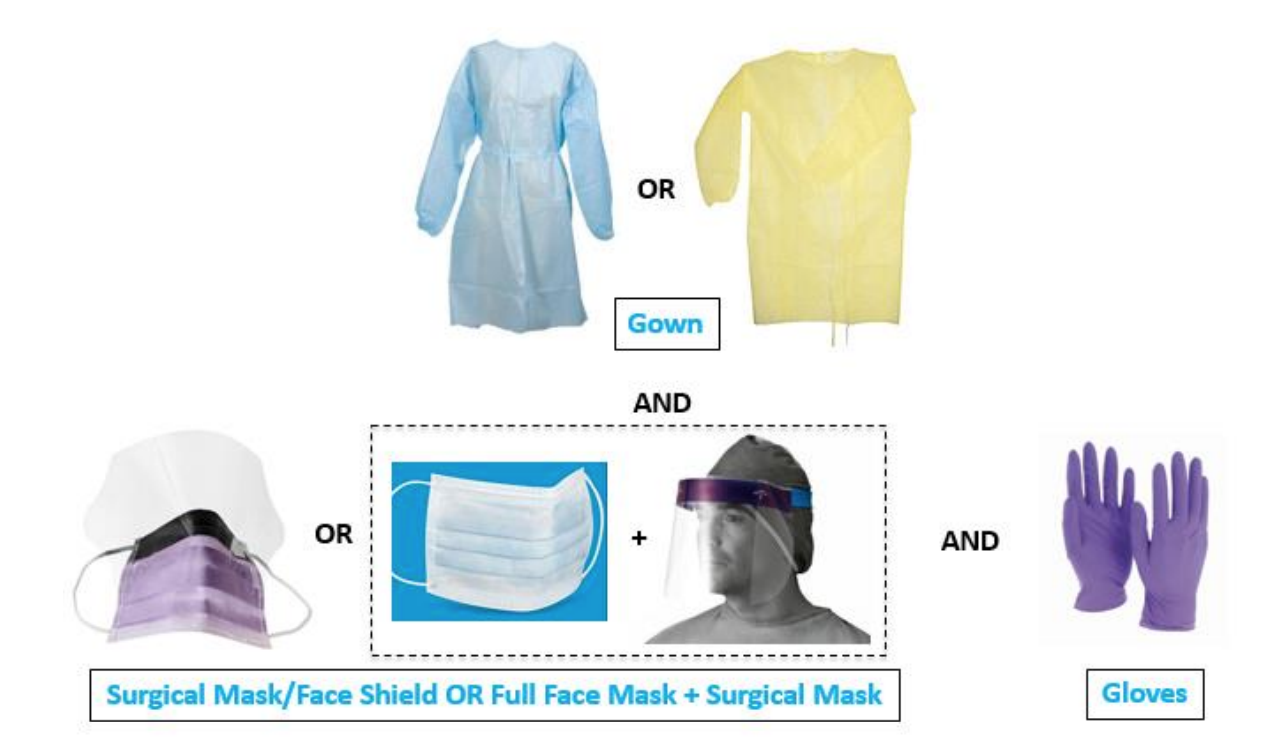
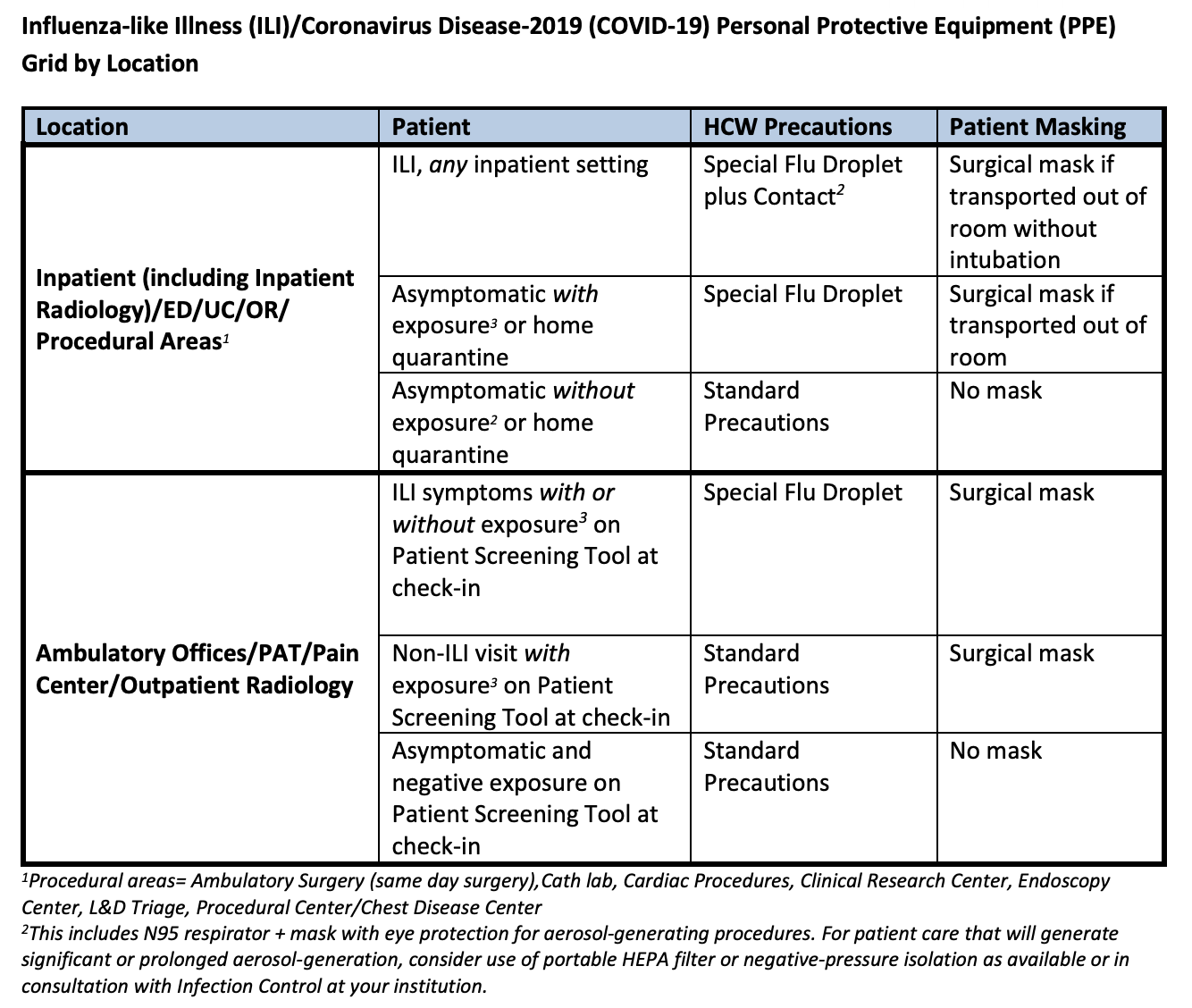
Healthcare organizations may further delineate the circumstances as to when which PPE is required. As an example of recommendations as of March 23 from [BILH Website](https://static1.squarespace.com/static/5c5b3374ca525b57bb9b3e4d/t/5e6992213d430e6e35aa5b99/1583976993771/BILH+COVID-19+PPE+Grid+by+Location.pdf) (with the important note that protocols are evolving rapidly), see chart below:
## Current Status/Shortage
As the COVID-19 outbreak continues to expand globally, the supply chain for PPE will continue to be stressed if demand exceeds available supplies ([FDA](http://www.fda.gov/medical-devices/personal-protective-equipment-infection-control/faqs-shortages-surgical-masks-and-gowns)).
The FDA [recommends strategies](https://www.fda.gov/medical-devices/letters-health-care-providers/surgical-mask-and-gown-conservation-strategies-letter-healthcare-providers) for use by healthcare organizations and personnel—categorized for a range of clinical needs and supply levels—to help determine conservation procedures during this time period. These strategies aim to augment, not necessarily replace, specific controls and procedures developed by health care organizations.
Due to shortages, new terminology is arising regarding extension or re-use of PPE:
**Extended Use:** wearing PPE without removal or redonning between patients.
**Re-Use:** removal and reuse of PPE between patients.
The current shortage has led many healthcare organizations to consider different avenues of conserving supplies to meet the needs of their staff, such as community donations. Furthermore, hospitals including Massachusetts General Hospital, Brigham and Women’s Hospital, and Beth Israel Deaconess Medical Center have instituted new policies, such as requiring universal face masks for all workers to be worn throughout the day for all cases, as the situation continues to evolve. See [current FDA recommendations](https://www.fda.gov/medical-devices/letters-health-care-providers/surgical-mask-and-gown-conservation-strategies-letter-healthcare-providers) for conservation recommendations for crisis situations.
*Thought questions:*
Your community hospital has been experiencing greater pressures on conserving the necessary protective equipment as well as personnel to help combat the virus. You receive an email requesting opportunities to help. Which PPE would the hospital need? What are some strategies to help provide enough protective attire to healthcare workers? What are some FDA approved alternatives/options?
## PPE Training
### Donning/Doffing PPE
These diagrams describe the application and removal of PPE. For a more comprehensive description and images of the types of PPE, please refer to Module 5 [Supplemental Material](https://docs.google.com/document/d/1bCEmruPePVoAe1CzY-g4Uuky-e5lOiCVJ4ywWL-X0jQ/edit): PPE. Note that in many hospitals, due to PPE shortage, masks, respirators, and eyewear are not discarded after single use (as shown in the figure), but are reused or used for an extended period of time. For example, partners' employees must wear face masks (surgical or procedural) at all times while in clinical care settings. In order to support the new policy, one surgical or procedural face mask will be issued at the start of each shift and will be used throughout the shift except in circumstances in which they become visible soiled or damaged (see next section for an example of reuse guidelines). Nonetheless, policies involving mask usage are constantly changing. A [new system](https://www.massgeneral.org/news/coronavirus/research/partners-healthcare-mask-sterilizing-facility) to sanitize up to 80,000 masks a day is currently underway and policies regarding its use are in development.


### Reusing PPE
Due to the limitations in supplies, many hospitals are creating new trainings concerning the reuse of PPE. PPE that was previously single-use only is now being reused. Contrary to the guidance from the above ‘doffing’ figures, surgical masks, N95 masks and eye protection are currently being reused to preserve hospital supplies.
The following is taught at the HMS/MGH PPE training session:
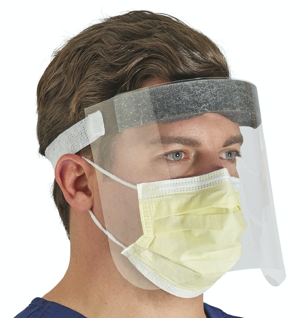
**Reuse of Face Shield**
The face shield is a good option for eye protection if you wear glasses. The exterior surface of the face shield is always considered contaminated. The interior surface is considered contaminated if it is worn over a mask or respirator that has been reused or is being worn under extended use.
1. Perform hand hygiene and don gloves.
2. With “clean hand,” hold mask by inside foam.
3. With “dirty hand,” clean interior and exterior surface of face shield using alcohol wipes or an alcohol prep. Do NOT use bleach wipes or Sani-Cloth, Virex, or other similar cleaners as these will cloud the clear plastic and make it difficult to see.
4. Remove gloves and perform hand hygiene.
**Reuse of Disposable Safety Glasses**
Disposable safety glasses consist of a plastic frame (blue section in picture) and an eye shield lens. The lens must be removed from the frame to adequately clean the glasses. This type of safety glasses can be worn over personal prescription glasses.

*Option 1: if replacement eye shields are NOT available*
1. Perform hand hygiene and don gloves.
2. Remove the eye shield lens from the frame.
3. Clean the eye shield with standard disinfectants and place in a clean area to dry.
4. Clean the frame with disinfectant wipes and place in a clean area to dry.
5. Remove gloves and perform hand hygiene.
6. Once dry, place the eye shield lens back onto the frame. Note: the eye shield must be inserted so that it lies behind the front of the frame.
*Option 2: If replacement lenses are available (currently NOT the case in most hospitals)*
1. Perform hand hygiene and don gloves.
2. Remove the eye shield lens from the frame and dispose of the eye shield.
3. Clean the frame with standard disinfectants. Allow the frame to dry following instructions on disinfectant wipe package.
4. Remove gloves and perform hand hygiene.
5. Obtain a new eye shield for the glasses and insert it onto the frame. Note: the eye shield must be inserted so that it lies behind the front of the frame.
**Reuse of Non-Disposable Safety Glasses**
Non-disposable safety glasses are meant to be reused. They cannot be worn over prescription glasses.

1. Remove eye protection by holding the the most posterior portion of the frames and lifting forward.
2. Wipe both surfaces of lenses with alcohol wipes or alcohol prep.
3. Wipe all other surfaces of the glasses with alcohol wipes or alcohol prep.
4. Perform hand hygiene upon exiting patient room
5. Glasses can be placed in any clean location for storage.
**Reuse of Surgical and N95 Masks**
1. Perform hand hygiene.
2. Carefully remove the mask from the face. Do NOT touch the exterior surface of the mask.
3. Place the mask in a container, such as a paper bag or plastic container, so that only the exterior surface of the mask is in contact with the container. Ensure that the elastic strap is placed to the side of the mask rather than lying inside the bag.
4. Perform hand hygiene.
**Donning a Reused Surgical or N95 Mask**
1. Perform hand hygiene and don gloves and gown.
2. Place the mask on the face, ensuring to only touch the outside of the mask and not your face with your hand.
3. Perform seal check (if using N95 mask).
4. Remove gloves and perform hand hygiene.
5. Don clean pair of gloves.
6. Don eye protection.
*Thought question:*
You volunteer at your medical school’s hospital and are asked to help train staff on how to reuse PPE. Think of up to five critical practices that all medical students need to know about reusing PPE.
## Frequently Asked Questions
**Which PPE should healthcare personnel wear when working with COVID-19 positive patients?**
As of April 25, 2019, the [CDC](https://www.cdc.gov/coronavirus/2019-ncov/infection-control/control-recommendations.html) recommends the following: As part of source control efforts, HCP should wear a facemask at all times while they are in the healthcare facility. When available, facemasks are generally preferred over cloth face coverings for HCP as facemasks offer both source control and protection for the wearer against exposure to splashes and sprays of infectious material from others. If there are anticipated shortages of facemasks, facemasks should be prioritized for HCP and then for patients with symptoms of COVID-19 (as supply allows). Cloth face coverings should NOT be worn instead of a respirator or facemask if more than source control is required. Nonetheless, any HCP who enter the room of a patient with known or suspected COVID-19 should adhere to Standard Precautions and use a respirator (or facemask if a respirator is not available), gown, gloves, and eye protection
**What PPE should patients with confirmed or suspected COVID-19 wear?**
Patients should wear nonsterile, disposable patient isolation gowns and should wear a facemask until they are isolated, whether that be in a hospital or at home. Once isolated, patients do not need to wear facemasks ([CDC](https://www.cdc.gov/coronavirus/2019-ncov/hcp/respirator-use-faq.html)).
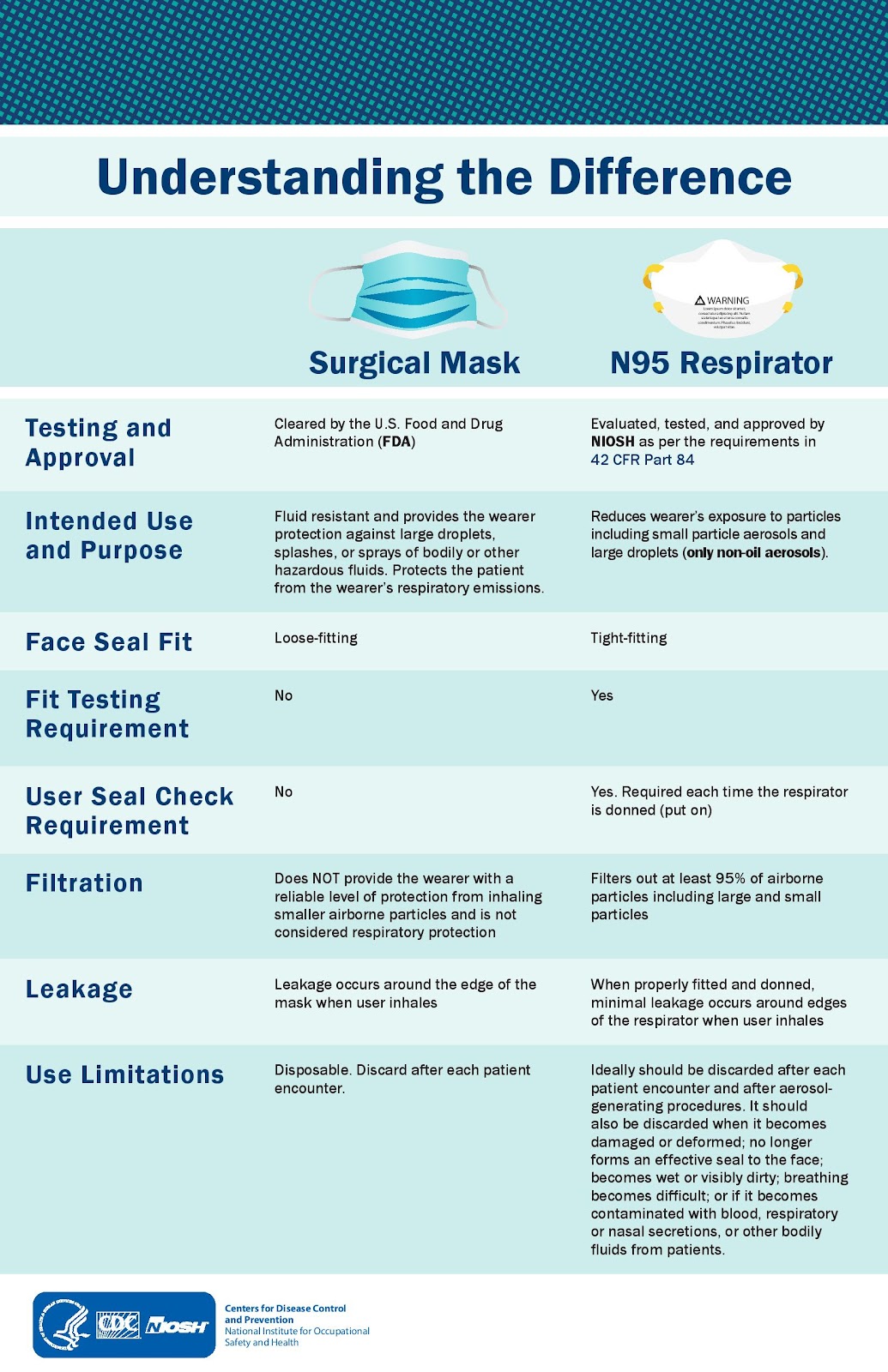
**What is the difference between an N95 respirator and a surgical facemask?**
An N95 respirator, which fits tightly to the face, filters at least 95% of small and large particles from the air, thus protecting users from airborne viruses. A surgical facemask, which fits loosely to the face, protects the user from large airborne droplets and splashes but does not prevent the inhalation of aerosolized virus particles ([CDC](https://www.cdc.gov/coronavirus/2019-ncov/hcp/respirator-use-faq.html#respirators)). See the figure below from the CDC: [Infographic - Understanding the Difference, Surgical Mask, N95 Respirator](https://www.cdc.gov/niosh/npptl/pdfs/UnderstandDifferenceInfographic-508.pdf).
**Which PPE is used in the following: Airborne Isolation/Droplet Isolation/Strict Isolation?**
Airborne Infection Isolation (“negative pressure”): N95 respirators.
Droplet Isolation: surgical and procedural masks
Droplet Isolation and Strict Isolation: Eye protection (face-shields and goggles)
**Who should be using PPE?**
According to the CDC:
* Patients with confirmed or possible SARS-CoV-2 infection should wear a facemask when being evaluated medically.
* Healthcare personnel should adhere to [Standard and Transmission-based Precautions](https://www.cdc.gov/coronavirus/2019-ncov/infection-control/control-recommendations.html) when caring for patients with SARS-CoV-2 infection.
* In light of new data about how COVID-19 spreads, along with evidence of widespread COVID-19 illness in communities across the country, CDC recommends that people wear a cloth face covering to cover their nose and mouth in the community setting. This is to protect people around you if you are infected but do not have symptoms.
**When should I use an N95 respirator vs. a facemask?**
Facemasks should be worn by patients with confirmed or suspected COVID-19 to prevent contamination when the patient coughs or sneezes. A facemask provides protection by containing droplets if someone has the virus and by preventing exposure to the virus if someone has close contact with another person who is infected. For healthcare personnel interacting with a patient with known or suspected COVID-19, the [CDC](https://www.cdc.gov/coronavirus/2019-ncov/infection-control/control-recommendations.html#adhere) recommends using an N95 respirator or a facemask if a respirator is unavailable. In addition, N95 respirators may be needed for clinical situations in which infectious droplets could become aerosolized, which occurs only in specific clinical situations such as when a patient is intubated. ([CDC](https://www.cdc.gov/coronavirus/2019-ncov/hcp/respirator-use-faq.html)). Practically, there is currently a shortage of N95 respirators, so many hospitals are recommending that healthcare personnel use regular facemasks, reserving N95 use for procedures in which aerosols could be generated. CDC provides guidelines for optimizing the supply of N95, which can be found [here](https://www.cdc.gov/coronavirus/2019-ncov/hcp/respirators-strategy/crisis-alternate-strategies.html).
**How do I make sure that my N95 respirator fits me correctly?**
All healthcare personnel should undergo formal mask fit testing prior to using an N95 respirator ([NIOSH](https://www.osha.gov/SLTC/etools/respiratory/respirator_basics.html#fit_testing)). This ensures there is an airtight seal between the healthcare worker’s face and the respirator. In addition, each time healthcare workers don an N95 respirator, they should perform a [user seal check](https://www.cdc.gov/niosh/docs/2018-130/pdfs/2018-130.pdf?id=10.26616/NIOSHPUB2018130) ([CDC](https://www.cdc.gov/coronavirus/2019-ncov/hcp/respirator-use-faq.html#respirators)).
**Does the universal mask policy apply to every member of the workforce working anywhere at Partners HealthCare and Beth Israel Deaconess Medical Center?**
The universal mask policy applies to employees working in buildings or areas (i.e., home care) where clinical care is provided or when walking through common areas in those same buildings.
* Workers in private individual offices or in nonclinical settings where individuals are reliably separated by more than 6 feet, do not need to wear the mask in those settings. When walking through common areas in buildings where care is delivered, however, the mask policy applies.
Workers that work in nonclinical buildings (i.e., Assembly Row) are excluded.
* These employees should practice principles of social distancing, respiratory etiquette and frequent hand hygiene.
* If these workers visit buildings where clinical care is provided, the mask policy applies as above.
**In procedural areas, can a single face mask be worn continuously, including across different cases?**
Yes, a single mask can be worn across different cases. Masks must be changed, however, if they become wet or contaminated during a case or a shift.
**I work in a clinical setting. How can I eat when I am supposed to wear a face mask (surgical or procedural)?**
Eating is not permitted in clinical areas. If you are working in a clinical setting, follow the removal and reuse instructions as is outlined in Partners Infection Control Guidance on Extended Use and Reuse.
**I work in a clinical setting. How can I drink when I am supposed to wear a face mask (surgical or procedural)?**
Drinking is permitted in designated locations in clinical areas. If you need to drink, ensure you are 6 feet away from others, perform hand hygiene, remove the mask, drink, and then replace your face mask.
**I work in a nonclinical setting. How can I eat and drink when I am supposed to wear a face mask (surgical or procedural)?**
Steps to remove mask in nonclinical settings, where eating/drinking is not restricted:
1. Perform hand hygiene with soap and water or an alcohol-based hand rub
2. Remove the face mask and place it on a clean surface such as a paper towel, paper bag or paper tray
3. Perform hand hygiene with soap and water or an alcohol-based hand rub before eating
Steps to replace mask after eating or drinking:
1. Put on face mask, taking care to avoid touching face or eyes
2. Perform hand hygiene with soap and water or an alcohol-based hand rub
**If I need to leave the facility and come back later in my shift, what should I do?**
Every effort should be made to limit exit and entry to the facility during your shift to preserve supplies of face masks. If you leave the facility, the face mask must be discarded and a new one obtained upon re-entry.
**Can I use my face mask between patients, including those with confirmed COVID-19, suspect COVID-19, other respiratory viruses or patients in whom none of these apply?**
Yes. Your face mask should be used according to the BIDMC guidelines and Partners Infection Control Guidance on Extended Use and Reuse, which ensures careful and deliberate handling of the mask to prevent both self-contamination and cross-contamination. Under conditions of extended use or reuse, a face shield is preferentially worn over the face mask as the form of eye protection.
**Should employees be wearing the mask at home and should their families wear masks?**
Employees should throw away their masks when leaving the hospital. They should not wear them home. There is generally no reason for employees and their families to wear masks at home. Social distancing and taking precautions like washing your hands, using hand sanitizer, and cleaning surfaces frequently should be appropriate for home. The Centers for Disease Control and Prevention (CDC) has provided this [guidance](https://www.cdc.gov/coronavirus/2019-ncov/prepare/prevention.html).
## Hospital-specific Policies
### Partners (BWH/MGH) Guidelines
MGH has published videos outlining and modeling the use reuse of [N95 respirators](https://youtu.be/IfTVPCDami4) and [surgical masks](https://youtu.be/JBq7TjIM5k0). For specific Partners guidelines, please follow [this link](https://pulse.partners.org/hub/departments/emergency_preparedness/coronavirus) (note: requires Partners credentials). These include recommendations for N95 respirators, surgical masks, and procedural masks, as well as eye protection.
### Beth Israel (BILH) Guidelines
Beth Israel has provided all guidelines under a [COVID-19 Information and Materials](https://www.bilh.org/covid19-information-assets) section of their website, updated frequently. Guidelines include [PPE recommendations](https://static1.squarespace.com/static/5c5b3374ca525b57bb9b3e4d/t/5e6992213d430e6e35aa5b99/1583976993771/BILH+COVID-19+PPE+Grid+by+Location.pdf) for providers and patients depending on location (inpatient vs ambulatory setting)
### Cambridge Health Alliance (CHA) Guidelines
CHA has provided all guidelines under a frequently updated [COVID-19 Quick Guide](https://sites.google.com/challiance.org/ncov-quick-guide/home), accessible with CHA credentials.
[Reuse policies](https://static1.squarespace.com/static/5c5b3374ca525b57bb9b3e4d/t/5e6da511ea160c0c82a63970/1584243985185/BILH+PPE+Reuse+Procedure+for+Respiratory+Evaluation+Units_Urgent+Care_Emergency+Department.pdf) for gowns, surgical masks, and eye protection. [Reuse instructions](https://covid-19.bilh.org/wp-content/uploads/2020/03/BILH-N95-Reuse-Procedure_3.18.20-2.pdf) for N95 respirators. [Reuse instructions](https://covid-19.bilh.org/wp-content/uploads/2020/03/BILH-Eye-Protection-Reuse-Guideline_3.20.20.pdf) for eye protection.
*Thought questions:*
* There is currently a supply shortage of many forms of PPE. How are CDC and hospital guidelines attempting to address this issue?
* Your family member asks you whether they should be wearing a mask to protect against coronavirus. How do you respond?
* You notice that members of the medical team in the hospital are not following hospital guidelines on appropriate use of PPE. As a medical student, what do you do?
---
# Agent Instructions: Querying This Documentation
If you need additional information that is not directly available in this page, you can query the documentation dynamically by asking a question.
Perform an HTTP GET request on the current page URL with the `ask` query parameter:
```
GET https://curriculum.covidstudentresponse.org/module-6-training-for-clinical-roles/personal-protective-equipment.md?ask=
```
The question should be specific, self-contained, and written in natural language.
The response will contain a direct answer to the question and relevant excerpts and sources from the documentation.
Use this mechanism when the answer is not explicitly present in the current page, you need clarification or additional context, or you want to retrieve related documentation sections.