# The Biopsychosocial Framework
To better understand how the pandemic may be causing this spike in mental health concerns, we are going to consider the cases of a new patient Adam as well as [Diane](https://curriculum.covidstudentresponse.org/curriculum-overview/cases) through the lens of the biopsychosocial (BPS) framework as well as the physiology of the trauma response. You’ve likely learned the BPS model in your past medical training, but if you want a refresher on the topic, you can review it [here](https://ajp.psychiatryonline.org/doi/abs/10.1176/ajp.137.5.535).
These cases capture some of the ways the pandemic may impact the mental health of our patients; we appreciate that there may be numerous factors that affect their health. Our goal is to demonstrate some of the prevalent stressors that we are seeing in our patients right now and provide examples of how to pull together the many interwoven life events that contribute to our patients' mental health.
## Adam’s Case
Let’s begin with Adam. Adam is a healthy, 20-year-old college student in Boston who has just returned to campus for his junior year.
Adam grew up outside of Seattle with his parents and older brother. He reports that he had a “happy childhood”, but that his high school years were challenging due to a tense relationship with his father. This relationship has further deteriorated during college because his father is constantly upset with Adam for spending his free time at parties with his friends from the soccer team, rather than focusing on his studies. Hanging out with his teammates both in practice and on the weekends has been Adam’s favorite part of college. Over the summer, Adam planned to live with friends while completing a prestigious summer internship. Within the space of a week in March, Adam’s second year of college came to an abrupt end and his plans for the summer were canceled. He had no other choice but to move back home to his childhood room and a tense environment with his father. In May, one of Adam’s grandmothers, a resident at an assisted care facility, passed away due to COVID. The family was unable to hold a funeral for her, and Adam feels like he was unable to adequately process his grief. The experience of losing his grandmother was a painful reckoning with the pandemic’s severity.
After five difficult months at home, Adam was eager to return to college for the fall term. Taking online classes at home in Seattle had proved difficult in the spring, and he felt that a return to campus would provide him with a more structured learning environment. He took difficult computer science classes and found himself struggling to learn the material without robust academic support. Even though his college mandated strict requirements about twice weekly COVID testing, and extracurricular activities (including his club soccer team) were limited, he was excited to spend time with his friends again in small groups.
Once Adam has arrived in his dorm, as he’s completing his mandated two-week quarantine, he sees on social media that a few of his friends living in off-campus housing have started to throw parties that are prohibited by university regulations. It all looks like a lot of fun--exactly what he had missed in all his months at home. No one else seems to be as isolated as he feels. Adam wants to complete his quarantine and be responsible about social distancing, but he feels frustrated that after his terrible summer, he could face administrative consequences for trying to blow off a little steam. He knows that even if he contracts COVID-19 and develops symptoms, they are likely to be mild. At the same time, he is keenly aware of the risks of spending time indoors with a large group of people. He can’t help but think of his grandmother. Still, the challenges of remote learning and lost socialization weigh heavily on him. Even once he completes quarantine, Adam is worried that he does not have much to look forward to. He ultimately decides to reach out for care via a telehealth provider.
Adam has a past psychiatric history of depression and was prescribed SSRIs for a year during high school. His family mental health history is notable for depression in his maternal grandmother, as well as anxiety and panic disorder in his mother. He denies tobacco or drug use.
*Thought Question:*
* What additional information have we missed here that you might want to help evaluate Adam’s current presentation?
## Adam's Biopsychosocial Formulation
What ***biological factors*** are contributing to Adam’s current presentation? In addition to his family history, which may genetically load him for mental illness, he has a personal history of depression. The COVID-19 pandemic has deeply affected many individuals, and young people seem to be at particular risk. One study found that while overall depression rates in the US rose from 8.7% the year of 2017-2018 to 10.6% by April 2020, the rates of depression in those aged 18-34 years old increased from 7.8% to 21.2% ([Daly et al., Journal of Affective Disorders 2020](https://www.sciencedirect.com/science/article/pii/S0165032720327609?via%3Dihub)). Of note, individuals with pre-existing substance use disorders may face additional burdens during this crisis. We will outline specific challenges that these individuals face in our at-risk populations sections.
Now, what ***psychological factors*** are contributing to Adam’s current presentation? There are many psychological factors and underlying personality vulnerabilities that could contribute to Adam’s current mental health status. One that is particularly relevant to the COVID-19 pandemic may be barriers to using previously formed **coping mechanisms**. Some of Adam’s existing coping mechanisms, such as playing soccer or spending time with friends, are now no longer available to him. Like Adam, many of our patients must now identify new coping mechanisms to help them deal with their day-to-day-stressors. Mental health can also affect one’s access to coping strategies: one survey conducted showed that those who self-identify as having depression also tend to report that they are less connected with family during the pandemic ([Costa et al., Psychiatric Services 2020](https://ps.psychiatryonline.org/doi/10.1176/appi.ps.202000245?url_ver=Z39.88-2003\&rfr_id=ori:rid:crossref.org\&rfr_dat=cr_pub%20%200pubmed)).
*Thought Question:*
* How would you coach Adam to consider additional coping mechanisms during the pandemic? If you want to learn more about a framework for thinking about coping mechanisms and stress during the pandemic, [here](http://researchgate.net/profile/Craig_Polizzi/publication/340515703_Stress_and_Coping_in_the_Time_of_COVID-19_Pathways_to_Resilience_and_Recovery/links/5e8e5acda6fdcca78901efbe/Stress-and-Coping-in-the-Time-of-COVID-19-Pathways-to-Resilience-and-Recovery.pdf) is a perspective piece that delves further into the issue.
In addition, Adam is now facing the psychological effects of **quarantine**, which are likely further exacerbating his presentation. A recent review of the mental health impact of quarantine during prior infectious disease outbreaks—including the 2003 SARS, 2010 H1N1, and 2014 Ebola outbreaks—suggested that individuals undergoing quarantine reported increased post-traumatic stress symptoms, confusion, and anger. Some of these effects may even be long lasting ([Brooks et al., Lancet 2020](https://www.thelancet.com/journals/lancet/article/PIIS0140-6736\(20\)30460-8/fulltext#bib5)). There were also social effects of quarantine. Quarantined healthcare workers continued to engage in avoidance behaviors following quarantine, including minimizing contact with patients ([Marjanovic et al., IJNS 2007](https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7094220/)). All of these sequelae are important to consider when caring for Adam both now and once the COVID-19 pandemic resolves.
What are the ***social contributors*** to Adam’s current presentation? From the vignette, it appears there are several. Like many individuals, he is facing increased tension with his family, particularly his father, with whom he was suddenly forced to live with again following the move to remote learning by colleges in the spring. He is also still processing the loss of his grandmother without the space to fully grieve, and is struggling with his own personal role in preventing the spread of COVID-19. Due to social distancing guidelines, in-person funerals and religious assemblies have been limited, which detracts from many people’s mourning process. Now, he is back on campus, which has unexpectedly exacerbated his feelings of isolation. Adam is conflicted as he chooses between safe quarantine protocols in his dorm and social connection through off-campus parties.
There are many changes in Adam’s life that threaten his mental health. However, as healthcare providers, we work with all patients - both with and without mental illness diagnoses - to support their own mental health. Telepsychiatry has blossomed during this pandemic, and work in this field may greatly increase accessibility to care ([Di Carlo et al, Int J of Clin Prac 2020](https://onlinelibrary.wiley.com/doi/10.1111/ijcp.13716)).
\
It will also be important to assess Adam’s risk for **self harm and suicidality**. During the pandemic, many risk factors for suicide have been increased, including social isolation, unemployment, and financial difficulty. Encouragingly, Google searches for phrases related to suicide are down, and those seeking mental health care are up ([Halford et al., PLoS One 2020](https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7380602/)). However, gun sales and background checks have greatly increased during the pandemic ([Mannix et al., Annals of Int Med 2020](https://annals.org/aim/fullarticle/2765237/coronavirus-disease-2019-covid-19-firearms-united-states-epidemic-suicide), [Lang and Lang, SSRN 2020](https://papers.ssrn.com/sol3/papers.cfm?abstract_id=3593956)). Given the known risk gun ownership on suicide and ongoing mental health stressors experienced by patients at this time, risk assessment is going to be of utmost importance in the months ahead.
## Diane’s Case
Now let’s start thinking about [Diane](https://curriculum.covidstudentresponse.org/curriculum-overview/cases). Remember, Diane is a 72-year-old woman who has COPD, heart failure, depression, and anxiety. She’s proud to live on her own in an independent living facility for the elderly in the middle of the city, and doesn’t like to ask other people for help. Early in the spring, she was cautiously running errands herself with a mask and a pair of gloves. As the summer starts, Diane is increasingly worn down from isolation. She finds herself frequently tearful, and has difficulty sleeping. Although she keeps in touch with her children via daily phone or video calls, it isn’t enough to ease her loneliness. At a friend’s suggestion, she meets up for “distanced” coffee at an outdoor restaurant. Feeling comfortable with how careful the servers seem to be, she starts to make plans to carefully resume some of her usual activities. Her children worry about her out in public--she lives in an area where COVID cases are rising-- and they tell her to isolate herself at home. However, Diane feels much less anxiety while interacting with her friends, and she tells her children that she’s taking adequate precautions.
In late June, Diane wakes up with a dry cough. She calls her PCP for a COVID test, which comes back positive. She becomes very worried about this diagnosis, and can’t tell when her breathlessness is due to COVID or a possible panic attack. Her anxiety is exacerbated by her children, who call incessantly to check in on her because she lives alone. After one phone call in which she was short of breath and dizzy while trying to talk, her daughter calls 911 and Diane is taken by ambulance to the hospital. On admission, Diane is found to have an oxygen saturation of 78 and a fever of 101.2. She’s placed on supplemental oxygen and is moved from the ED to a COVID unit. Her family video chats and calls her while she’s in the hospital, but Diane is often confused as to who they are and where she is. Her breathing becomes increasingly labored over the course of a week, and she is sedated and intubated.
The rest of her hospital stay is a blur. She does not remember being weaned off the ventilator a month later, nor does she remember the transfer to rehab. Diane is at the rehabilitation center for about two weeks before returning home. However, as September starts, Diane still doesn’t feel like herself. Besides her physical weakness, residual dry cough, and easily-induced shortness of breath, she finds non-physical tasks also difficult. She finds it hard to think through steps for simple things she used to do without issue, like making breakfast. Diane suspects it could be her lack of good sleep. Her family continues to call, but she hardly has the energy for more than a 2 minute conversation. This is a large change from how she felt in June, when she felt very energetic and enthused to see friends. Diane has also stopped returning her friends’ calls. This is in part due to fatigue but also because she has heard that another friend in her circle also contracted COVID, and she feels guilty that she didn’t take the pandemic as seriously as she should have. Diane finds herself waking up in the middle of the night with her heart racing, and has a hard time recognizing her room for about a minute once she wakes up. In addition, she is unusually tired during the day. Napping doesn’t provide her the rest she thinks it should. Recently, she received a large medical bill for her time in the ICU and her rehab center, which is much more than what she feels she can afford, particularly right now. Even though money is tight, she still relies on delivery services for her groceries when she cannot get out of bed. It’s now been about 10 weeks since her hospitalization. She has stopped trying to guess when she will feel better again.
She presents to her PCP for “exhaustion.” Notes from her two follow-up appointments after her discharge from rehab focus on her residual dry cough and fatigue; she missed her third follow-up appointment altogether. Today, when she comes to the office, Diane’s hair and clothing are disheveled. She has been using a walker since her hospitalization and moves very slowly. Diane reports that she has been taking her SSRI, but that it doesn’t “seem to be helping at all.” She feels as though she is still sick and that she has not yet recovered.
## Diane’s Biopsychosocial Formulation
What ***biological factors*** are contributing to Diane’s current presentation? Diane’s age, coupled with additional risk factors such as COPD and heart failure, place her in a high risk category for a protracted disease course following exposure to COVID-19. Unfortunately, she experienced severe symptoms of COVID-19, including fever and shortness of breath, and required **intubation**. Fatigue and continued shortness of breath were demonstrated by 72% and 65% of COVID-19 survivors respectively 29-70 days after ICU discharge ([Halpin et al., Journal of Medical Virology 2020](https://onlinelibrary.wiley.com/doi/full/10.1002/jmv.26368)). Physical difficulties, such as weakness, can also persist long after ICU stays. A cluster of physical, psychological and cognitive symptoms known as **post-intensive care syndrome (PICS)** could also be contributing to Diane’s exhaustion. Physically, this could include weakness and reduced exercise tolerance, although this could be confounded in Diane’s case with long-lasting symptoms of COVID-19. A small study of about 150 patients in Rome surveyed an average of about 60 days following onset of COVID-19 symptoms found that only 12.6% of patients were free of symptomatology. Even those that did not require hospitalization reported continued fatigue, dyspnea, and chest pain ([Carfi et al,JAMA 2020](https://jamanetwork.com/journals/jama/fullarticle/2768351)).
What psychological factors are contributing to Diane’s current presentation? In addition to the physical contribution of PICS, many of the symptoms patients experience after a long course in the ICU are psychiatric in nature. PICS, on top of her current fatigue and uncertainty of when or if she will ever feel better, may have contributed to the worsening of her **depression**. There are elements of her nightmares that could indicate development of **PTSD**, another common finding in patients with PICS ([Lane-Fall et al,. Anesthesiology Clin 2019](https://www.anesthesiology.theclinics.com/article/S1932-2275\(18\)30099-5/fulltext)). As many as 80% of patients with PICS also have some amount of **cognitive impairment**. Diane’s stay in the hospital introduced a number of risk factors for the psychological sequelae of PICS, including a poor recollection of events in the ICU, delirium (could not recognize her family over video, nor remember where she was), and a long period of ICU sedation ([Biehl and Sese, Clev Clin J Med 2020](https://www.ccjm.org/content/early/2020/07/29/ccjm.87a.ccc055.long)).
Lastly, what ***social factors*** are contributing to Diane’s current presentation? Early in the pandemic’s course, Diane was isolated from her support network, and found herself tearful and frustrated at simple tasks. She had great anxiety surrounding her errands for which she had to leave the house. However, as restaurants started opening their doors for customers, Diane found that seeing her friends for lunch contributed a great deal to her mental health and life satisfaction. She prioritized this in the wake of her intense loneliness. Following her COVID-19 infection, Diane blames herself for getting sick and possibly exposing others. In part, this **guilt** prevents her from reaching out and developing her social support from afar. Support from her family is also limited, as they live far away and cannot contribute to physical errands. Compounding her isolation, guilt, and anxiety are the medical bills for a hospital stay she does not remember. Her **financial obligations** add to her anxiety, as she is retired with limited savings. Financial strain and employment status have been shown to worsen depression ([Zimmerman & Katon, Health Econ 2005](https://onlinelibrary.wiley.com/doi/abs/10.1002/hec.1011)). Any prospect of working to help pay off her medical debt is out of the question: her fatigue and cognitive impairment prevent her from doing anything more than the bare minimum to maintain herself.
*Thought questions:*
* Thinking specifically about Diane’s cognitive impairments, what factors besides those above could be contributing? Fit these factors into your own biopsychosocial framework.
* In what ways has Diane’s hospitalization changed her independence at home?
### COVID-19 as Traumatic Exposure
Above, we discussed how COVID-19 dramatically changed Adam and Diane’s daily lives. For them and for many patients, the pandemic and its consequences may represent significant traumatic exposures. Trauma is defined by the Substance Abuse and Mental Health Services Administration (SAMHSA) as “an event, series of events, or set of circumstances that is experienced by an individual as physically or emotionally harmful or life threatening and that has lasting adverse effects on the individual’s functioning and mental, physical, social, emotional, or spiritual well-being” ([SAMHSA 2014](https://ncsacw.samhsa.gov/userfiles/files/SAMHSA_Trauma.pdf))
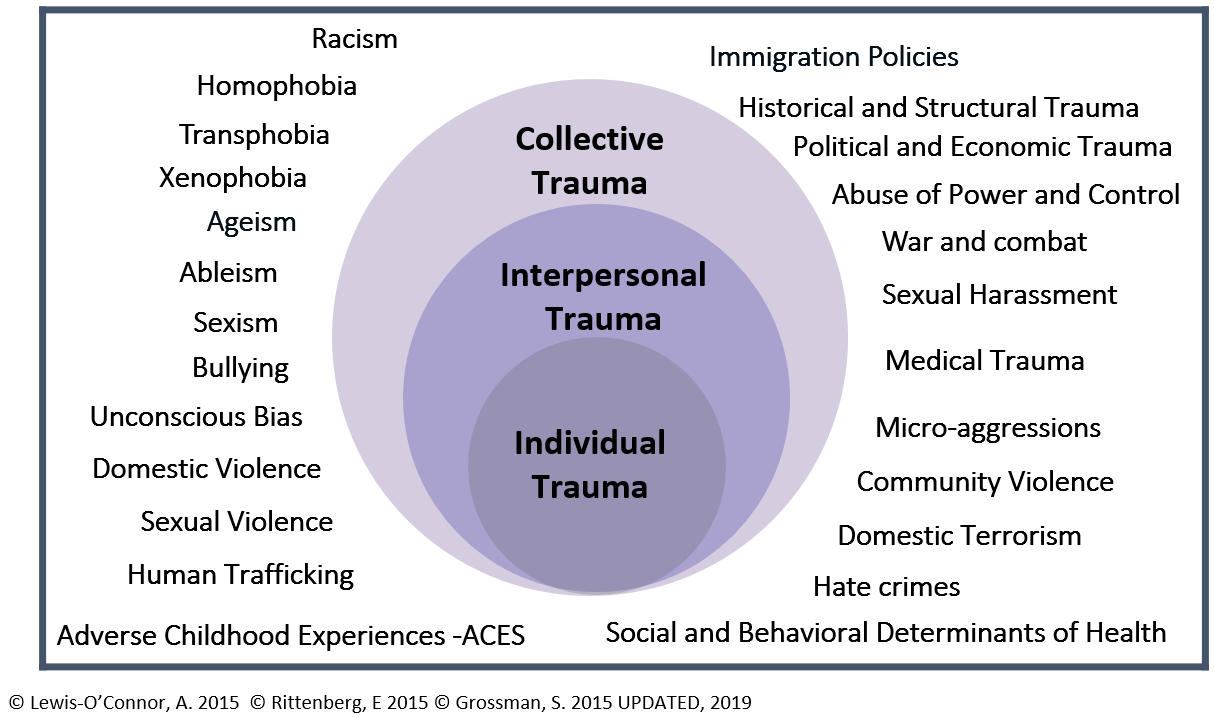
Traumatic exposures may occur at an individual, interpersonal, or collective level, as shown in the figure below. The pandemic may affect individuals at any or all three levels. At the individual level, for example, Diane is suffering from a long and protracted hospital course, as well as perhaps long-term COVID-19 symptoms, and has lost the independence she so valued. At the interpersonal level, Adam experiences a deterioration of his relationships with friends and family. At the collective level, Adam and Diane are constantly exposed to the illnesses of those around them as well as a societal grappling with deaths and other losses.
The experience of trauma has been documented to impact mental and physical health across the life-course. In the landmark [Adverse Childhood Experiences study](https://www.ajpmonline.org/action/showPdf?pii=S0749-3797%2898%2900017-8), childhood exposures to trauma were linked with adult health outcomes such as depression, substance use disorders, and cardiovascular disease in a dose-dependent fashion. The mechanism by which trauma leads to poorer health outcomes is still under investigation, but is thought to be mediated by neurohormonal and metabolic adaptations to stress that change both physiology and behaviors ([McEwen, JAMA 2017](https://jamanetwork-com.ezp-prod1.hul.harvard.edu/journals/jamapsychiatry/fullarticle/2619523)).
Module 6 addresses how the traumatic exposure of COVID-19 is doubly burdensome for healthcare providers, as well as approaches to mitigate those impacts and skills to care for yourself and those around you.
## **Review**
To review, in this section we have discussed the biological, psychological, and social forces that contribute to worsening mental health outcomes during the COVID-19 pandemic. They include:
* Biological: age, heightened stress response, coexisting medical and psychiatric comorbidities, prolonged ICU stays and personal illness due to COVID-19
* Psychological: changes in available coping skills, quarantine increasing feelings of anger and confusion, anxiety and guilt of contracting the illness, traumatic exposures
* Social: financial insecurity, changes to family dynamics, loss of social networks and community supports, additional weight of caring for others who are suffering.
*Thought Questions:*
* This list is far from complete. What other factors do you think are playing a role at this time?
* How might a personal history of trauma impact the mental health needs of our patients now and the health needs of our population in the long term?
---
# Agent Instructions: Querying This Documentation
If you need additional information that is not directly available in this page, you can query the documentation dynamically by asking a question.
Perform an HTTP GET request on the current page URL with the `ask` query parameter:
```
GET https://curriculum.covidstudentresponse.org/module-4-mental-health-in-the-time-of-covid-19/the-biopsychosocial-framework.md?ask=
```
The question should be specific, self-contained, and written in natural language.
The response will contain a direct answer to the question and relevant excerpts and sources from the documentation.
Use this mechanism when the answer is not explicitly present in the current page, you need clarification or additional context, or you want to retrieve related documentation sections.